How we help
Everbridge digitizes organizational resilience at scale and enables customers to protect their people and assets with an integrated suite of critical event management solutions.
Everbridge named a Leader in The Forrester WaveTM: Critical Event Management Platforms, Q4 2023. We empower organizations to anticipate, mitigate, respond to, and recover stronger from critical events. Our unified platform digitizes organizational resilience, achieving the highest score possible in 15 criteria including orchestration and automation, according to Forrester’s report.




Everbridge 360™ represents our relentless dedication to provide our customers with the most comprehensive and unified interface to manage critical events across one single platform so you can know earlier, respond faster, and improve continuously.
More effectively manage critical events, minimize communication delays, and improve overall organizational resilience through the industry’s most advanced and unified dashboard.
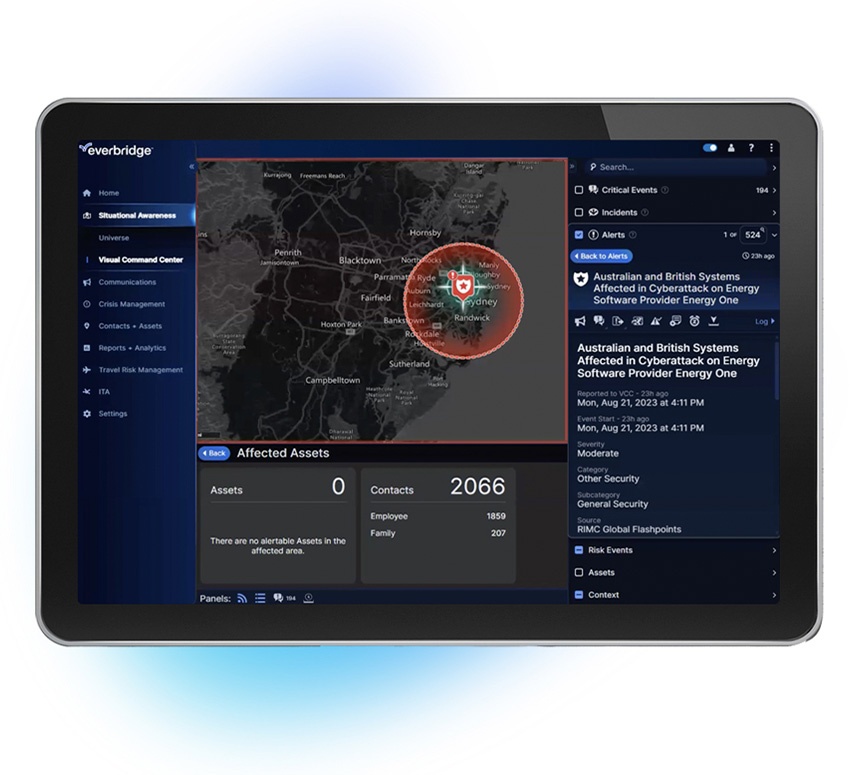
Everbridge digitizes organizational resilience at scale and enables customers to protect their people and assets with an integrated suite of critical event management solutions.

As a mission-driven organization, Everbridge is committed to fulfilling our duty of care, guiding our customers through critical challenges, and positively impacting the world. Our customers include Fortune 1000 businesses, and leaders in industries such as: financial services, healthcare, tech and telecom, energy and utilities, transportation, retail and eCommerce, government, manufacturing, and education.

“With the Crisis Management module, we’re able to quickly assess the situation, activate the appropriate plan, and ensure the right actions are being taken to best protect our people and our branches.”
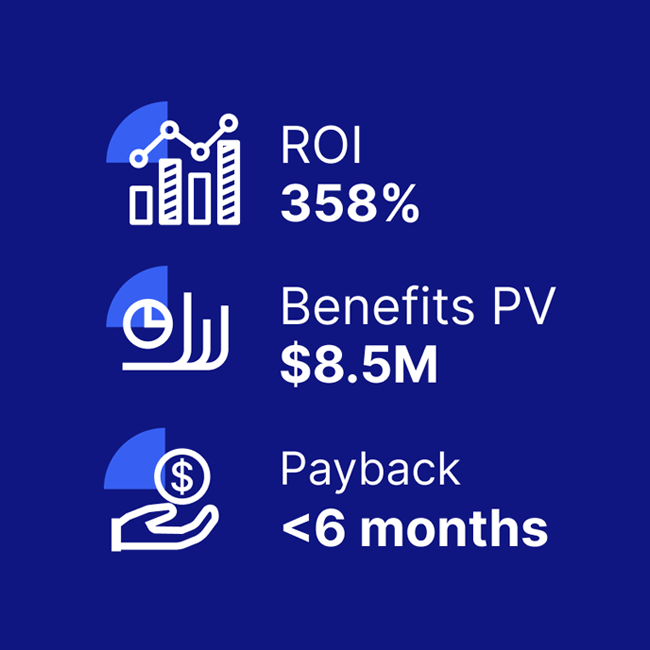
A composite organization comprised of interviewees with experience using the CEM platform achieved a 358% ROI and US$8.5M in three-year risk-adjusted benefits, according to a commissioned Total Economic Impact(TM) Study by Forrester Consulting.
This includes:
Discover the value Everbridge can bring to your organization from our ROI calculator, checklist, and full TEI study.